What Does “Immediate Action” Mean on NCLEX?
Do you aspire to crush NCLEX questions concerned with patient stability? Then you must understand the concept of immediate action in clinical situations that demand urgent intervention
When you sit for your licensure exam, you are essentially entering a simulated environment where time is your most precious resource. The phrase immediate action on NCLEX does not merely refer to doing something quickly; it represents the precise moment where a clinician must intervene to halt a downward physiological spiral. Recognizing this threshold is what separates an entry-level practitioner from a student, as it demonstrates the ability to distinguish between chronic discomfort and acute crisis.
Your primary objective in any nursing scenario is to maintain or restore patient stability. In the context of the exam, a stable patient is one whose compensatory mechanisms are still functioning effectively, whereas an unstable patient is actively failing. This guide will dismantle the cognitive architecture behind urgent decision-making, providing you with a sophisticated lens through which to view every "first action" prompt you encounter.
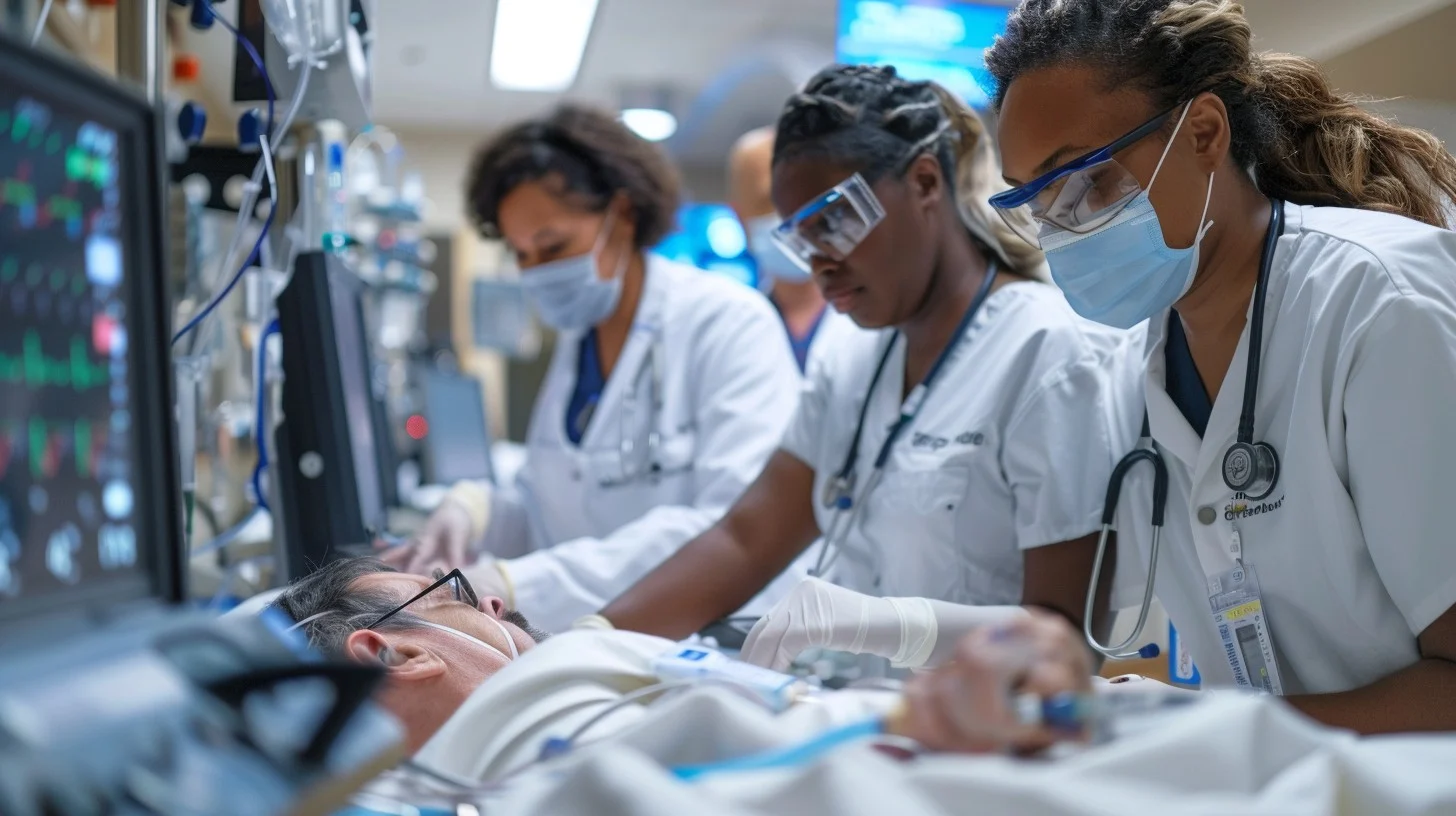
Hands down, shifting your perspective from "task completion" to "clinical triage" is essential for long-term testing success. So, you must learn to look past the superficial details of a case study and identify an intervention that serves as the final barrier between a patient and a medical emergency. By embracing the concept of immediate action on NCLEX, you position yourself as a safe, vigilant advocate capable of managing the most volatile clinical environments.
Whether you aspire to become an RN or an LPN, read on to understand the nitty-gritty of immediate action on NCLEX.
The Physiology of Urgency: Beyond the Basics
Identifying Failure to Rescue
One of the most significant professional benchmarks in modern healthcare is the prevention of failure to rescue. This term describes the inability of a clinician to recognize and respond to early signs of deterioration, a theme that heavily influences immediate action on NCLEX scenarios. This benchmark tests your ability to spot the "red flags" in vital signs or lab data that signal an impending loss of patient stability before it becomes irreversible.
Evaluating the ABC Hierarchy with Sophistication
While every student learns the Airway, Breathing, and Circulation (ABC) hierarchy, the exam requires a more nuanced application of these principles. Immediate action on NCLEX often involves identifying which of the three is under the most direct threat in a specific patient population. For instance, while a breathing issue is generally a high priority, an active arterial bleed, which is a circulation crisis, may require your hands-on intervention even before addressing a minor respiratory distress.
A patient receiving an intravenous (IV) infusion of an antibiotic suddenly reports a "tight feeling" in the throat and develops audible wheezing. After stopping the infusion, which action should the clinician perform next?
The Role of Rapid Assessment in Crisis
In many urgent scenarios, the required action is a targeted physical assessment to confirm a suspected complication. However, when a patient's patient stability is visibly crumbling, the immediate action on NCLEX pivots from data collection to life-saving implementation. Understanding when to stop assessing and start acting is the hallmark of professional maturity. For this reason, this understanding is frequently tested in NCLEX questions.
Pharmacological Priorities and Urgent Response
Recognizing Anaphylaxis and Acute Reactions
Medication safety is a massive component of the NCLEX, specifically regarding the recognition of adverse physiological events. When a patient shows signs of a systemic allergic reaction, the immediate action on NCLEX is always the cessation of the offending agent. Protecting patient stability in this context means acting within seconds to prevent the closure of the airway or a total circulatory collapse.
A clinician receives a laboratory report for a patient showing a serum potassium level of 6.5 mEq/L. Which intervention is the priority?
High-Alert Medications and Targeted Interventions
Administering potent substances like insulin, heparin, or potassium requires a constant state of vigilance. If a patient receiving a high-alert medication begins to show signs of toxicity, your immediate action on NCLEX must be the implementation of the specific reversal protocol. This often involves a delicate balance between pharmacological knowledge and the rapid-fire prioritization needed to maintain the patient's neurological and cardiac integrity.
The Intersection of Labs and Action
Laboratory results often serve as the catalyst for an urgent nursing response. If you receive a critical lab value that threatens patient stability, such as a potassium level of 6.2 mEq/L, your immediate action on NCLEX is rarely to "recheck the result." Instead, you should immediately initiate cardiac monitoring and prepare to administer stabilizing agents to protect the heart from lethal arrhythmias.
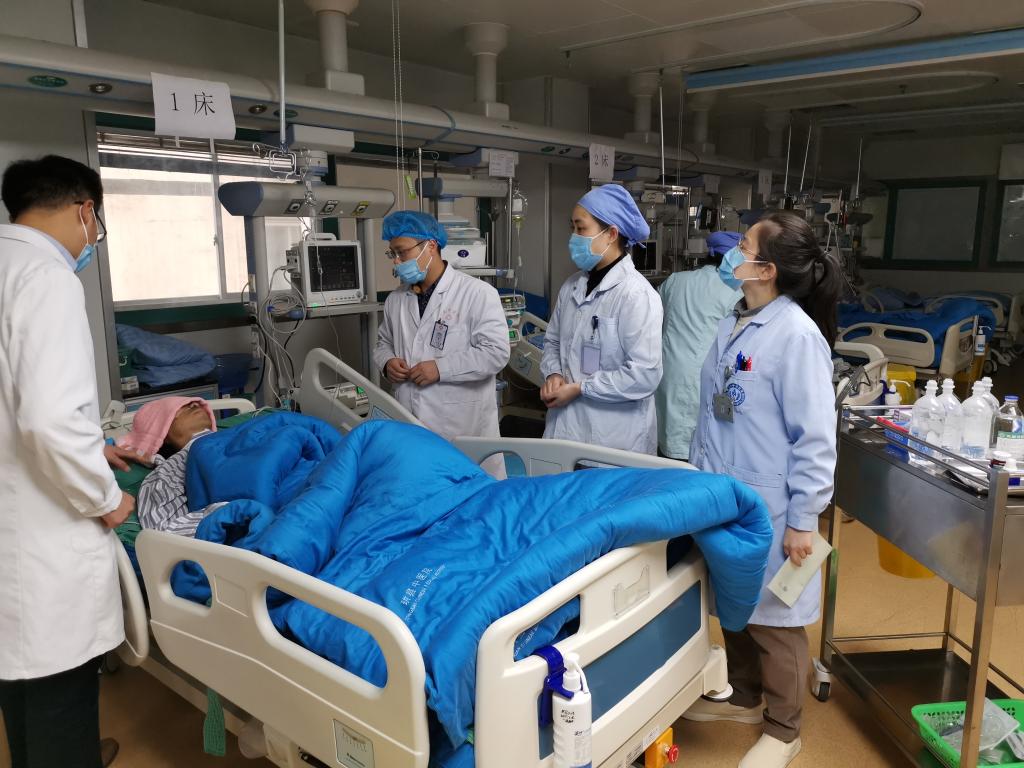
Surgical and Post-Operative Vigilance
Detecting Early Hemorrhage
The post-operative period is a minefield of potential complications that require a rapid response. When a patient’s blood pressure begins to trend downward while their heart rate climbs, the immediate action on NCLEX is to assess the surgical site for signs of occult bleeding. Maintaining patient stability in a post-surgical environment requires you to be two steps ahead of a potential hypovolemic shock scenario.
While performing a neurological check, the nurse notes that a patient who was previously alert is now difficult to arouse and has a newly unequal pupil size. What is the most appropriate immediate action?
Evisceration and Wound Dehiscence
Certain surgical emergencies require a very specific, manual immediate action on NCLEX that defies standard task-based logic. If a wound eviscerates, your priority is not to call the surgeon first, but to protect the exposed organs with sterile, saline-soaked dressings. This physical intervention is the only way to preserve tissue viability and maintain the patient's overall stability until they can be returned to the operating suite.
Neurological and Sensory Emergence
The "Time is Brain" Philosophy
Neurological changes are among the most subtle yet devastating shifts a nurse can witness. In immediate action on NCLEX questions involving potential strokes or increased intracranial pressure, your response must be guided by the time is brain philosophy. Rapidly identifying a change in the level of consciousness is the most critical step in preserving long-term patient stability and preventing permanent disability.
A patient with a 10-year history of Chronic Obstructive Pulmonary Disease (COPD) is receiving oxygen at 2L via nasal cannula. The latest arterial blood gas (ABG) shows a PaCO2 of 70 mmHg and a pH of 7.28. Which interpretation is correct?
Managing Seizure Activity and Safety
When a patient experiences a seizure, the immediate action on NCLEX focuses entirely on the protection of the airway and the prevention of physical injury. You must resist the urge to restrain the patient or to insert objects into the mouth, as these actions directly threaten the patient's stability. Instead, you demonstrate your clinical competence by turning the patient to their side and timing the event to ensure a safe recovery phase.
Tactical Pitfalls: What to Avoid in Urgent Scenarios
The Fallacy of Chronic Normalization
A common mistake on the exam is normalizing a dangerous lab value because the patient has a chronic condition. For example, while a patient with COPD may have a higher baseline CO2, a sudden spike that leads to respiratory acidosis still demands immediate action. So, never allow a chronic diagnosis to blind you to an acute threat to the patient's stability.
Distinguishing Between "First" and "Best"
Many students struggle with differentiating between the "first" action and the "best" long-term plan. In immediate action on NCLEX prompts, the "first" action is the one that addresses the most immediate threat to life. While several options may be "correct" in a general sense, the priority answer stabilizes the patient right now, leaving the secondary tasks for after the crisis has passed.
The Significance of Decisive Clinical Response
Cultivating Clinical Intuition
Developing a command over immediate action on NCLEX is about more than just checking boxes; it is about building the intuition that saves lives. When you can look at a complex set of data and instinctively know which intervention restores patient stability, you have transitioned from a novice to a competent professional. This intuitive leap is what the licensure exam is designed to measure.
The Ethical Weight of Rapid Response
Your duty as a clinician involves the ethical obligation to provide timely and effective care. By becoming proficient in immediate action on NCLEX, you are fulfilling your professional promise to act as a guardian for those in your care. This commitment to maintaining patient stability is the foundational principle of the nursing profession and the key to your success on the exam.
Elevate Your Testing Performance on NCLEX
At this juncture, you can effectively identify and respond to urgent scenarios in the exam. By viewing every question through the lens of immediate action on NCLEX, you can bypass the distractors and focus on the intervention that truly matters. This approach will help you synthesize data and act decisively to maintain the highest standard of patient stability.
As you continue your preparation, remember that every "immediate action" you analyze is a skill you will carry into the hospital. Thus, success with immediate action on NCLEX is the ultimate validation of your readiness to enter the profession. To perform exemplarily in the upcoming NCLEX, keep your focus on the patient, prioritize the most acute risks, and you will emerge from the exam as a safe, capable, and licensed professional.



No comments yet. Be the first to comment!